Can You Be Allergic to Dental Fillings?
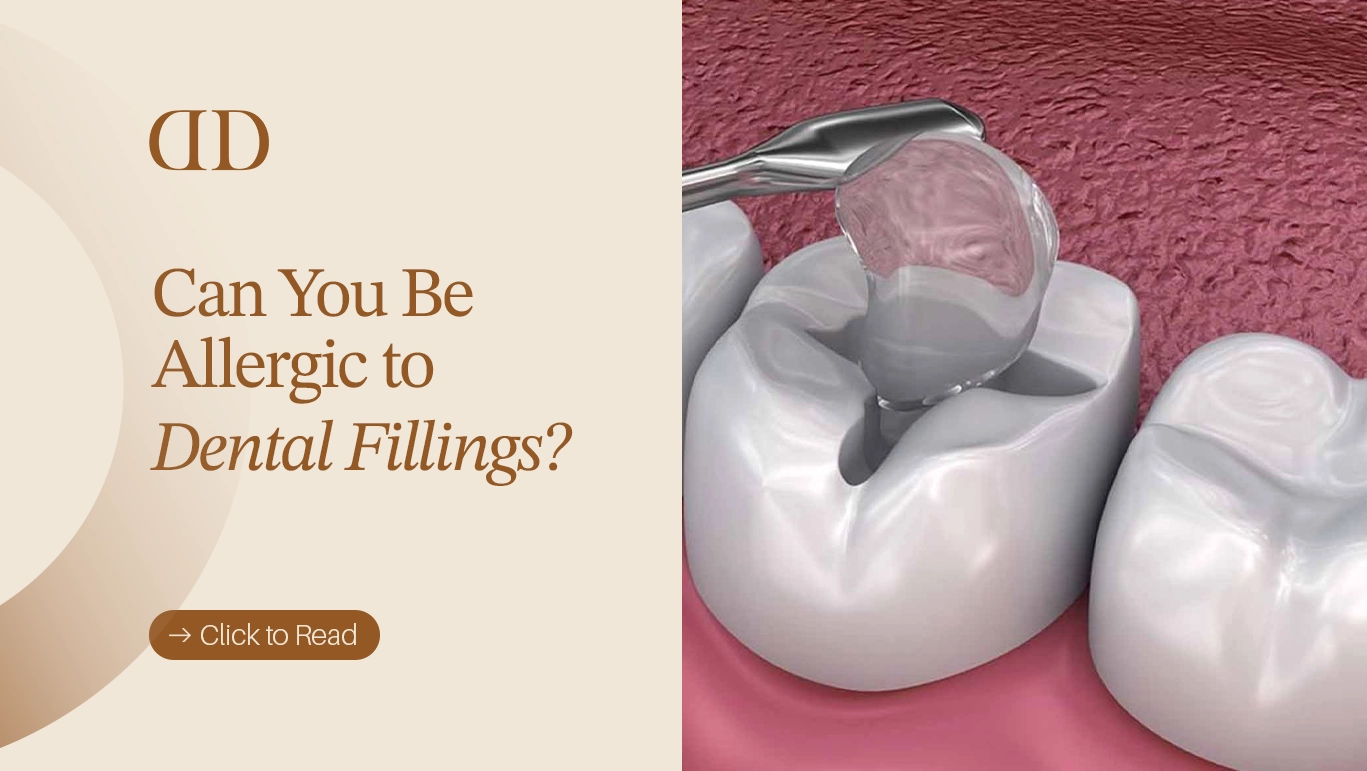
Allergic to dental fillings is a question that sounds rare, almost niche, yet it quietly concerns thousands of people who experience unexplained symptoms after dental work. Tingling lips, a metallic taste that won’t fade, persistent gum irritation, or even headaches can make patients wonder whether their dental filling is truly harmless. While most people tolerate fillings without any issues, sensitivity and allergic reactions are real topics of discussion in modern dentistry.
At Darya Dental Clinic, patients often arrive with similar concerns: “Can i be allergic to dental filling materials?” The short answer is that reactions are uncommon, but not impossible. More importantly, these reactions can look very different from classic allergies, which is why they are frequently misunderstood or misdiagnosed.
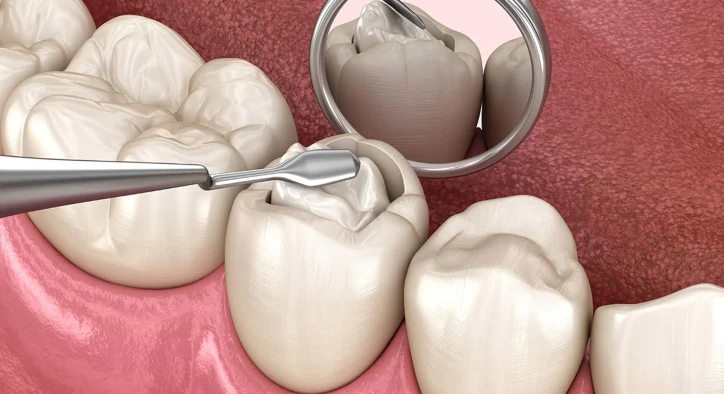
Can I Be Allergic to Dental Filling?
The idea of being allergic to dental fillings may sound surprising because fillings are designed to be biocompatible. They are tested, regulated, and used on millions of patients every year. However, the human immune system is complex, and what is neutral for one person may trigger sensitivity in another.
An allergic to dental fillings materials usually involves a delayed immune response rather than an immediate one. This means symptoms might appear days or even weeks after the procedure, making the connection harder to recognize. Patients sometimes attribute discomfort to stress, oral hygiene changes, or unrelated health issues.
It is also important to distinguish between true allergy and material sensitivity. A true allergy involves an immune response, while sensitivity may be a localized irritation or intolerance. Both can feel similar, but their underlying mechanisms differ. In discussions about allergic to dental fillings, this distinction is often overlooked, leading to confusion online.
From a clinical perspective, reported reactions are rare. Large-scale reviews referenced by organizations like the American Dental Association suggest that adverse reactions occur in a very small percentage of patients. Still, “rare” does not mean “impossible,” and that’s where personalized dental care becomes relevant.
For readers interested in broader scientific context, the American Dental Association provides material safety discussions here: American Dental Association – Dental Materials
Types of Fillings and Possible Allergic Reactions
Understanding whether someone is allergic to dental fillings starts with understanding what fillings are made of. Each material interacts with oral tissues differently, and each has its own risk profile.
Dental fillings are not a single category. They range from metal-based alloys to tooth-colored resins and glass-based compounds. Because of this variety, an allergic reaction to dental filling materials is often material-specific rather than a blanket reaction to “fillings” as a whole.
Premium Dental Care in Turkey
Expert treatments with high-end technology. Get your personalized quote today via WhatsApp.
Below is a simplified overview of commonly used filling types and how they may relate to sensitivity or allergy discussions.
Amalgam Fillings
Amalgam fillings have been used for over a century and contain a mixture of metals, including mercury, silver, tin, and copper. Discussions about being allergic to dental fillings often start here because metals are known allergens for some individuals.
In rare cases, patients report oral lichenoid reactions localized lesions near amalgam restorations. These reactions resemble oral lichen planus and are believed to be contact reactions rather than systemic allergies. Scientific literature suggests that removing or replacing amalgam sometimes resolves symptoms, though evidence varies case by case.
It’s worth noting that most people with amalgam fillings experience no adverse effects at all. Large population studies have not established widespread harm, but individual sensitivity remains a topic of ongoing research.
Composite Resin Fillings
Composite resin fillings are popular due to their natural appearance. However, when people describe an allergic reaction to dental filling, composites are increasingly part of the conversation.
These materials may contain methacrylates or other resin-based compounds. In dental professionals, skin contact allergies are better documented, while patient reactions are far less common. Still, some patients report burning sensations or gum irritation near resin restorations.
Because composite fillings are bonded directly to tooth structure, distinguishing between bonding irritation and true allergy can be challenging. This ambiguity is one reason why allergic to dental fillings discussions require careful, individualized evaluation rather than assumptions.
Ceramic (Porcelain) and Gold Fillings
Ceramic and gold fillings are often considered more inert. Gold, in particular, has a long history of use in dentistry. True allergy to high-purity gold is extremely rare, but trace metals in alloys may cause reactions in sensitive individuals.
Ceramic materials are generally well tolerated and often chosen for patients with known metal sensitivities. In conversations about allergic to dental fillings, these materials are frequently mentioned as alternatives rather than causes.
Glass Ionomer Fillings
Glass ionomer fillings release fluoride and chemically bond to tooth structure. They are often used in pediatric or preventive dentistry. Reports of an allergic reaction to dental fillings involving glass ionomers are very limited, but mild tissue irritation has been observed in some cases.
Because these materials are less complex chemically, they are often considered low-risk in terms of allergic potential. However, as with all dental materials, individual responses can vary.
Why Individual Response Matters
What makes the topic of allergic to dental fillings so complex is that reactions are not solely about materials. Oral environment, saliva composition, immune sensitivity, and even stress levels can influence how the body responds.
Research summaries from institutions such as the National Institutes of Health highlight that oral mucosal reactions are multifactorial and not always linked to a single cause: National Institutes of Health Oral Mucosal Reactions
This is why blanket statements rarely apply. Two patients with identical fillings may have completely different experiences.
What to Do If You Suspect Allergic to Dental Fillings
Suspecting that you may be allergic to dental fillings often begins with subtle signals rather than dramatic symptoms. A persistent burning sensation, unexplained gum redness, or discomfort that lingers long after the filling has settled can raise questions. These signs are rarely definitive on their own, which is why many people spend months searching for explanations unrelated to dentistry.
One important point is timing. An allergic reaction to dental filling materials is often delayed. Unlike classic allergies that appear within minutes, oral reactions may develop gradually. This delay complicates self-observation and makes cause-and-effect harder to establish. Patients frequently report that symptoms “feel dental” but are inconsistent enough to cause doubt.
When people start asking whether they are allergic to dental fillings, documentation becomes valuable. Keeping notes about when symptoms appear, whether they worsen during chewing, or if they are localized near a specific tooth can help frame more productive conversations. While this is not diagnostic, it supports clearer communication and avoids vague descriptions.
Clinics with experience in international and complex cases, such as Darya Dental Clinic,
often emphasize careful listening over immediate conclusions. Rather than assuming a filling is the cause, dentists typically consider bite issues, nerve sensitivity, existing oral conditions, or stress-related habits that may mimic an allergic reaction to dental fillings.
Another layer of complexity is differentiating oral allergy from systemic reactions. Most reported cases related to allergic to dental fillings remain localized in the mouth. Widespread symptoms are far less common and usually prompt investigation beyond dentistry alone.
Observation Before Action
Before any changes are considered, observation plays a central role. Many symptoms attributed to allergic to dental fillings resolve on their own as tissues adapt. The mouth is a dynamic environment, and healing responses can look alarming before they normalize.
Scientific discussions in dental journals frequently caution against immediate removal of restorations without clear evidence. Unnecessary replacement may introduce new materials and new uncertainties. This conservative approach is supported by reviews such as those summarized by the British Dental Journal, which highlight the importance of differential diagnosis in suspected dental material reactions: British Dental Journal – Dental Material Sensitivities
Testing and Material Awareness
In some cases, patch testing or material history reviews are discussed when allergic reaction to dental filling concerns persist. These methods are imperfect and do not always translate directly to oral tissues, but they may offer context rather than answers.
Awareness is often more impactful than testing alone. Knowing whether you have reacted to metals, resins, or certain cosmetics in the past can inform future dental conversations. This background helps frame whether concerns about being allergic to dental fillings are plausible or coincidental.
Importantly, most people who question an allergic reaction to dental filling never receive a definitive confirmation. Instead, they gain reassurance, alternative explanations, or a better understanding of how their mouth responds to change.
How to Prevent the Need for Fillings Altogether
While discussions about being allergic to dental fillings are important, many readers are equally interested in avoiding fillings entirely. Prevention shifts the focus away from materials and toward habits, environment, and timing.
Cavities develop over time, and early-stage enamel changes are often silent. By the time a filling is needed, the process has already progressed. Understanding this timeline reframes prevention as a long-term strategy rather than a quick fix.
From a scientific perspective, prevention does not guarantee freedom from dental work, but it can reduce frequency and complexity. This indirectly lowers the chances of ever questioning whether you are allergic to dental fillings in the first place.
Everyday Habits and Risk Awareness
Dietary patterns, saliva composition, and oral hygiene routines interact in complex ways. Research consistently shows that frequency of sugar exposure matters more than quantity. This insight helps explain why some people develop cavities despite brushing regularly.
For individuals concerned about allergic reaction to dental fillings, prevention can feel empowering. Fewer restorations mean fewer material interactions and fewer unknowns. Even partial risk reduction can be meaningful over decades.
Regular assessments also play a role. Early detection may allow for non-invasive monitoring rather than immediate restoration. While this approach is not always possible, it reflects a broader shift toward conservative dentistry.
Material Conversations as Part of Prevention
Prevention is not only about avoiding decay; it also includes informed choices when treatment becomes unavoidable. Discussing material options in advance helps align expectations and reduces anxiety around allergic to dental fillings concerns.
Modern dentistry offers more alternatives than ever before. Even when fillings are required, material selection can be individualized. This flexibility is one reason why fears surrounding allergic reaction to dental fillings have become less prominent in recent years.
Preventive strategies are widely discussed in global oral health research, including reports by the World Health Organization that emphasize education and early intervention as core pillars of oral health: World Health Organization – Oral Health
Bringing It All Together
The question “Can you be allergic to dental fillings?” does not have a simple yes-or-no answer. The reality sits somewhere in between certainty and speculation. Being allergic to dental fillings is possible, but rare, and often difficult to confirm.
What makes this topic compelling is not fear, but nuance. Dental materials have evolved significantly, patient awareness has grown, and conversations between patients and clinicians are more detailed than ever. This combination has transformed what was once a fringe concern into a legitimate, if still uncommon, topic of interest.
Ultimately, discussions about allergic reaction to dental filling are less about materials alone and more about listening to symptoms, to timing, and to the broader context of oral health. When approached thoughtfully, these conversations empower patients to engage with dentistry not as passive recipients, but as informed participants.
FAQ About Allergic to Dental Filling
Questions about being allergic to dental fillings tend to surface long after the dental visit itself. Unlike immediate pain or visible complications, suspected reactions often feel vague, delayed, and difficult to explain. This final section brings together the most common concerns people raise when trying to understand whether a filling could be the source of ongoing discomfort.
Rather than offering definitive answers, these FAQs reflect patterns seen in patient narratives, clinical discussions, and published observations. The goal is clarity, not certainty.
Can an allergic reaction to dental filling appear years later?
One of the most confusing aspects of being allergic to dental fillings is timing. Many people assume that if a reaction were going to happen, it would appear immediately. In reality, some reported reactions develop slowly or become noticeable only after changes in oral conditions.
Scientific literature suggests that delayed hypersensitivity reactions are possible, especially when oral tissues are repeatedly exposed to the same material over long periods. However, it is equally important to note that age-related gum changes, new medications, or altered bite forces can create symptoms that resemble an allergic reaction to dental filling without being one.
This overlap is why late-onset discomfort is often investigated cautiously rather than attributed directly to fillings.
Are metal fillings more likely to cause allergic reactions than white fillings?
When people search for allergic to dental fillings, metal fillings often dominate the conversation. This is partly because metals such as nickel are known allergens in other contexts, like jewelry.
Amalgam fillings contain multiple metals, and localized oral reactions near these restorations have been documented. However, composite (white) fillings are not completely free from discussion either. Resin-based materials contain organic compounds that can also trigger sensitivity in rare cases.
In other words, the question is less about “metal versus white” and more about individual response. No single material can be labeled universally risky or universally safe in the context of allergic reaction to dental fillings.
Can symptoms of being allergic to dental fillings mimic other oral problems?
Yes, and this is one of the biggest challenges. Symptoms associated with allergic to dental fillings such as burning mouth sensation, gum irritation, or metallic taste overlap with many non-allergic conditions.
Dry mouth, nutritional deficiencies, stress-related clenching, and even hormonal changes can create sensations that feel alarming but are unrelated to filling materials. This overlap often explains why people cycle through multiple explanations before considering an allergic reaction to dental filling.
Understanding this mimicry helps explain why dentists are careful not to rush to conclusions based on symptoms alone.
Is removing a filling the only solution if allergy is suspected?
Removal is often seen as the obvious solution when someone believes they are allergic to dental fillings, but it is rarely the first consideration in clinical discussions.
Replacing a filling introduces a new material, a new bonding process, and new variables. In some reported cases, symptoms improved after replacement; in others, they remained unchanged. This mixed outcome highlights why removal is considered a last step rather than a default response.
Modern dentistry emphasizes evaluation and monitoring before intervention. Clinics that focus on patient-specific planning, such as Darya Dental Clinic, often frame filling replacement as one option among many, not an automatic fix.
For readers interested in how professional organizations view this topic, the American Academy of Oral Medicine provides insights into oral mucosal reactions that are often mistaken for allergies: American Academy of Oral Medicine – Oral Reactions
How common is it to be truly allergic to dental fillings?
Despite widespread online discussions, true allergy remains uncommon. Large reviews indicate that confirmed immune-mediated reactions to dental materials affect a very small percentage of patients.
This does not invalidate personal experiences. Instead, it suggests that being allergic to dental fillings is the exception rather than the rule. Many cases fall into a gray area of sensitivity, irritation, or coincidence rather than confirmed allergy.
Understanding this context can reduce anxiety while still validating the need for thoughtful evaluation.
